ODAC Dermatology, Aesthetic & Surgical Conference’s Medical Director, Dr. Adam Friedman, discusses the ODAC 2021 program, reasons to attend and more!
To view the full agenda, click here: https://staging.orlandoderm.org/agenda/
ODAC Dermatology, Aesthetic & Surgical Conference’s Medical Director, Dr. Adam Friedman, discusses the ODAC 2021 program, reasons to attend and more!
To view the full agenda, click here: https://staging.orlandoderm.org/agenda/

Source: The Dermatologist
The following is an excerpt from The Dermatologist as coverage from ODAC Dermatology, Aesthetic & Surgical 2020 where Sailesh Konda, MD, and Vishal Patel, MD, reviewed the guidelines and discussed considerations for when and when not to perform MMS.
Mohs micrographic surgery (MMS) is considered the gold standard of treatment for many skin cancers. However, this option is not always appropriate for every situation and every patient. Several factors should be considered when determining which option to use, including tumor size, patient age, and aesthetic outcomes, for treating skin cancer.
The Dermatologist: What are the guidelines for determining what tumors should and should not be treated with MMS?
Dr Konda: The appropriate use criteria (AUC) for MMS was developed in 2012 by an ad hoc task force.2 In general, MMS may be considered as a treatment option for tumors on the head, neck, hands, feet, pretibial surface, ankles, and genitalia; aggressive tumors of any location; tumors greater than 2 cm on trunk or extremities; recurrent tumors, and tumors arising in patients with a history of immunosuppression, radiation, or genetic syndromes.
An AUC score is assigned to tumors based on their characteristics. Tumors with scores of 7 to 9 are appropriate, 4 to 6 are uncertain (in extenuating circumstances, MMS may be considered), and 1 to 3 are inappropriate.
However, practitioners should remember that these are only guidelines! Even if a tumor meets criteria for MMS, the physician and patient should still discuss all available treatment options—both surgical and nonsurgical— and take into consideration associated cure rates; long-term clinical and aesthetic outcome; the patient’s age and comorbidities; and risks, benefits, and adverse effects before deciding on a treatment.
The Dermatologist: What tumors often deemed appropriate for MMS might not actually require MMS, and why?
Dr Konda: Superficial basal cell carcinoma and squamous cell carcinoma in situ are tumors that have been deemed appropriate for MMS. However, these tumors may also be treated with topical therapy (imiquimod and 5-fluorouracil), local destruction, fusiform or disc excision, photodynamic therapy, and lasers (CO2 +/- diode for follicular extension). These treatment modalities may provide cure rates lower than but approaching those of MMS, and may be preferred by physicians and patients in certain circumstances. When discussing treatment options, patients should be made aware of any therapies that may be used off-label or are not FDA-approved.
Additionally, lentigo maligna (melanoma in situ) and lentigo maligna melanoma may be treated with either MMS (frozen sections), staged excision with central debulk and complete margin assessment (permanent sections), or wide local excision (permanent sections).

Source: Next Steps in Derm
Backed by a mountain of evidence, Dr. Zitelli walked us through the new and changing role of sentinel lymph node biopsy for melanoma in a riveting 20-minute talk presented at the 16th annual ODAC conference. Here are the highlights.
Before delving in, Dr. Zitelli skillfully laid the framework for his lecture. The crux of sentinel lymph node biopsy is based on the theory of orderly progression, in which malignant melanoma cells leave the tumor and preferentially enter the lymphatics and the first lymph node. This theory is rivaled by the anatomic pathway, in which malignant melanoma cells may enter the lymphatics or the blood stream, resulting in simultaneous dissemination.
The overwhelming preponderance of evidence supports the latter anatomic theory – melanoma cells may enter the blood stream directly or the lymphatics, potentially bypassing the sentinel node. This anatomic theory is evidence based. It refutes the theory of orderly progression that the concept of sentinel lymph node biopsy is based on. Another common misconception is that lymph nodes are filters – they are not. Lymph nodes are sampling organs, sampling antigens in order to initiate an immune response.
With the groundwork laid, Dr. Zitelli went on to summarize the emerging evidence for sentinel lymph node biopsy. “This is what you need to know when you counsel a patient in order to obtain true informed consent.”
What you’ve been told: Sentinel lymph node biopsy improves survival
What the evidence shows: There is not a single solid tumor for which sentinel lymph node biopsy has been shown to provide a survival benefit.
We’ve been told that sentinel lymph node biopsy improves survival in intermediate thickness melanoma, because subclinical deposits are removed from the lymph nodes before they can grow. In fact, 33% of patients who underwent sentinel lymph node biopsy, did so because they thought it would improve their survival. Yet, there is not a single solid tumor – melanoma, gastric, renal, thyroid or otherwise – where electively removing normal lymph nodes, even in the case of microscopic involvement, has shown a survival benefit.
A cornerstone trial, the Multicenter Selective Lymphadenectomy Trial (MSLT-1), set out to prove the survival benefit of sentinel lymph node biopsy in melanoma. However, sentinel lymph node biopsy failed to improve melanoma specific survival. Subsequently, MSLT-2 looked at whether removing positive lymph nodes further down the line would improve survival in patients who had positive sentinel lymph nodes – this was also a negative study.
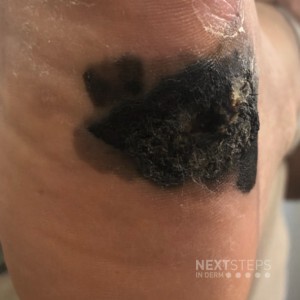
Source: Dermatology Times
Sentinel lymph node biopsy (SLNB) has classically been performed for regional disease control and to hopefully prevent disease metastasis; however, according to one expert, there has not been any good evidence to support this practice. As such, it is important for clinicians to focus on the evidence when planning the treatment and management of their advanced melanoma patients.
“Over the last decade or so, the role of SLNB has been changing, and there is no real consensus as to when to perform the procedure because it is a very rapidly changing field. The touted usefulness in survival benefit or prognosis of SLNB simply cannot be backed up by the available data, essentially rendering the appropriate use of SLNB in therapeutic limbo,” said John Zitelli, M.D., clinical associate professor, departments of dermatology & otolaryngology, University of Pittsburgh Medical Center, Pittsburgh, Penn., who spoke at the Orlando Dermatology and Aesthetic Conference.
According to Dr. Zitelli, the theory that SLNB would provide a survival benefit was debunked with the MSLT-1 research study1 recently published in the New England Journal of Medicine, and the idea that the procedure was to be considered as the most accurate prognostic test was also shown to be untrue. There usually is no need to do a SLNB, Dr. Zitelli said. The Breslow thickness, as well as all of the presenting clinical pathological morphologic features, such as ulceration of the tumor, is a wealth of information that the clinician can use to contemplate appropriate further treatment and management of the patient. Many clinicians still prefer to perform SLNB, Dr. Zitelli said, reasoning that waiting until the tumor is palpable would likely be synonymous with greater complications.
“The premise is off, because if you’re performing SLNB on a lot of people and the complication rate is low but the number of patients who are getting the procedure is high, the long-term complication rate in a group of people who you manage with SLNB actually have more complications than the smaller group of patients who have a complete node dissection from palpable disease,” Dr. Zitelli said.
Controversy revolving around the role of SLNB and its true usefulness in melanoma therapy and management continues today. The current contemporary wisdom is that SLNB should be performed because the results could help determine which patients would be more amenable to adjuvant therapy.

Source: Dermatology Times
The Orlando Dermatology Aesthetic & Clinical Conference (ODAC), formerly known as Orlando Derm, is scheduled for January 18-21 at the JW Marriott in Orlando.
This year’s meeting will open with presentations from physicians who will address advances in treating skin of color, hot topics in surgical dermatology and cutaneous malignancy, the latest on photodynamic therapy, and a year in review from the Journal of Drugs in Dermatology, among others.
Drs. Eric Bernstein and Jason Pozner will host a panel discussion on “My Top Picks for Laser and Energy Based Treatments.” And, Dr. Joel Cohen will give an overview of facial arterial supply.
During the general session on Saturday, Jan. 19, Dr. Brian Berman will address managing urticaria, which will be followed by talks by Dr. Deirdre Hooper on platelet rich plasma for hair growth and skin rejuvenation; Dr. Andrew Alexis on keloids and disorders of hyperpigmentation in skin of color; and, Drs. Bernstein and Pozner will address advances in non-surgical skin tightening.
On Sunday, January 20, Dr. Jean Bolognia will open the day’s general session with a review of advances in systemic therapies for melanoma.
For more information, visit ODAC online at https://staging.orlandoderm.org.

Source: Dermatology News
Another reason not to prescribe opioids for postoperative pain – besides potentially adding to the epidemic the nation – comes from evidence showing these agents can impair wound healing.
In addition, epidermal sutures to close dermatologic surgery sites may be unnecessary if deep suturing is done proficiently. These and other pearls to optimize wound closure were suggested by Robert S. Kirsner, MD, PhD, professor and chair of the department of dermatology and cutaneous surgery at the University of Miami.
Avoid opioids for postoperative pain
“We know the opioid epidemic is a big problem. An estimated 5-8 million Americans use them for chronic pain,” Dr. Kirsner said at the Orlando Dermatology Aesthetic and Clinical Conference. “And there has been a steady increase in the use of illicit and prescription opioids.”
Emerging evidence suggests opioids also impair wound healing (J Invest Dermatol. 2017;137:2646-9). This study of 715 patients with leg ulcers, for example, showed use of opioids the most strongly associated with nonhealing at 12 weeks. “We found if you took an opioid you were less likely to heal,” Dr. Kirsner said. They found opioids significantly impaired healing, even when the investigators controlled for ulcer area, duration, and patient gender.

Source: Dermatology Times
Options for repairing nasal defects after skin cancer surgery should be based on location, size and depth of the defect, as well as patient preference.
“If the defect is centrally located in the alar groove, you may want natural healing to occur,” says Joel L. Cohen, M.D., associate clinical professor of dermatology at the University of Colorado in Denver, and director of AboutSkin Dermatology in Greenwood Village and Lone Tree, Colo. He spoke with Dermatology Times prior to his presentation on skin cancer nasal reconstruction at the recent Orlando Dermatology Aesthetic & Clinical Conference (ODAC) in Miami.
“In such a case, the natural concavity is often recapitulated by simply letting the skin granulate, without the need for any sutured repair.”
However, in many instances of nasal reconstruction, dermatologists have to decide which procedure will achieve the best aesthetic outcome and also, the level of wound care that can be managed by the patient.

Source: Dermatology News
In his practice, Joel L. Cohen, MD, spends a good part of his day doing Mohs surgery, “with the goal of cancer removal, and after surgery, having the patient look good,” he said at the Orlando Dermatology Aesthetic and Clinical Conference.
“Having resurfacing in my practice has allowed me to treat not only wrinkles and etched lines, but also help skin cancer patients by blending and minimizing their skin cancer scars,” said Dr. Cohen, an aesthetic dermatologist and Mohs surgeon in private practice in Denver.
For example, one of his patients was a kindergarten teacher who had a large rotation flap scar on her cheek after excision of a melanoma in situ. The children asked her about it all the time during the 2 months after the surgery, and she decided to come in for some laser sessions. “With three ablative fractional laser sessions, she really looked great just 3 months later and wasn’t even interested in wearing makeup at that point.”
Resurfacing in his practice using a variety of lasers is very helpful, Dr. Cohen said. He published a study in November that compared pulse dye laser, CO2 ablative fractional lasers, or a combination of both for modification of scars following Mohs surgery (J Drugs Dermatol. 2016 Nov 1;15[11]:1315-9).
The prospective, multicenter study revealed that although both monotherapy approaches were safe and effective, the combination of pulse dye laser and fractional ablative laser offered some synergy that was preferred by patients.

ODAC Dermatology, Aesthetic & Surgical Conference 2024
Physician Continuing Medical Education - AMA (MDs, DOs)
The Postgraduate Institute for Medicine designates this enduring material for a maximum of 27.5 AMA PRA Category 1 Credits™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Continuing PA Education - AAPA
Postgraduate Institute for Medicine has been authorized by the American Academy of PAs (AAPA) to award AAPA Category 1 CME credit for activities planned in accordance with AAPA CME Criteria. This activity is designated for 27.5 AAPA Category 1 CME credits. PAs should claim only the credit commensurate with the extent of their participation.
Continuing Nursing Education - ANCC (RNs, APRNs, NPs)
The maximum number of hours awarded for this Continuing Nursing Education activity is 27.5 contact hours. Nurses should claim only credit commensurate with the extent of their participation in the activity
Joint Accreditation Statement

In support of improving patient care, this activity has been planned and implemented by the Postgraduate Institute for Medicine and National Medical Education Corporation. Postgraduate Institute for Medicine is jointly accredited by the Accreditation Council for Continuing Medical Education (ACCME), the Accreditation Council for Pharmacy Education (ACPE), and the American Nurses Credentialing Center (ANCC), to provide continuing education for the healthcare team.
